1) Introduction
2) Neuro Institute (USA)
3 Project Walk (USA)
4) Coordination Dynamics Therapy (Estonia,
Spain)
5) Activity-Based Restoration (USA)
6) Beyond Therapy (USA)
7) Center SCI Recovery (USA)
8) Centro Giusti (Italy)
1)
Introduction: In recent
years, aggressive physical rehabilitation programs have emerged that seem
to restore significant function in many with SCI, even years after injury.
Sophisticated devices and technology have been developed to cat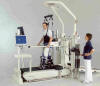 alyze
such function-restoring rehabilitation, such as GIGER-MD®
locomotion system (www.gigermd.com) or the Locomat® robotic
treadmill training (photo) (www.hocoma.com).
alyze
such function-restoring rehabilitation, such as GIGER-MD®
locomotion system (www.gigermd.com) or the Locomat® robotic
treadmill training (photo) (www.hocoma.com).
Frequently, these programs are used to maximize
restored function after an innovative surgical procedure or other
intervention. Often videos are created to document the patient’s
functional improvement, and given the impressive nature of the physical
activities that could be done after but not before treatment, it is
assumed that the recovered ability documents efficacy.
However, this assumption may or may not be valid. It
is possible that little of the restored function is due to, for example, a
$50,000 surgery but rather attributed to the rehabilitation aggressively
pursued after the surgery but not before. If functional recovery after a
surgical intervention depends upon a slowly regenerating neuron reaching
an anatomically distant target site, it will take a relatively long time
for new functional improvements to appear. If during that period, the
patient has sustained an aggressive physical rehabilitation program, it is
not unreasonable to question, as many scientists, indeed, do, what is the
true cause of the improvement. Because of this concern, some surgical
interventions are now requiring patients to aggressively rehabilitate
before the surgical intervention as well as after.
Furthermore, if a patient believes with
heart-and-soul conviction that the surgery/intervention will help him
recover some function, it will shift his consciousness from the
pre-surgical “you-will-never-walk-again” attitude that is often imprinted
on patients by medical authorities to a self-fulfilling belief of what may
be truly possible if he works hard . The patient’s will propels him to new
levels of function, much of which, in fact, may have little to do with the
surgery/intervention.
Even considering it alone without any potentially
confounding intervention, physical rehabilitation is a complicated area in
which observed improvement may be due to a number of causes separately or
in combination. First, through a variety of physiological mechanisms,
including growth-factor stimulation, aggressive physical rehabilitation in
many individuals with SCI probably does trigger some neuronal
regeneration.
Second, it may activate dormant but intact neurons
that transverse most injury sites, even in injuries clinically classified
as complete. Studies suggest that only a small percentage of “turned-on”
neurons are needed to regain significant function.
Third, the spinal cord in itself possesses
intelligent and not completely subservient to brain oversight.
Specifically, the spinal-cord’s “central-pattern generator” can sustain
lower-limb repetitive movement, such as walking, independent of direct
brain control. With training and appropriately designed leg braces,
impressive ambulation may be observed with minimal if any neuronal
regeneration.
Fourth, many muscles above the injury site affect
ambulatory potential, especially when using appropriately designed leg
braces. For example, the latissimus dorsi, a muscle innervated from the
spinal-cord’s cervical region, can influence pelvic-area movement and, in
turn, ambulatory-associated motions (Anton Wernig, private communication).
Fifth, increasingly, many scientists believe that
there are intriguing possibilities about the integration of different
neurological systems above and below the injury site, which, although
making our understanding of the nervous system more complicated than once
assumed, generate rehabilitation opportunities.
Sixth, aggressive physical rehabilitation programs
are often initiated relatively soon after injury in a period in which
there is already appreciable recovery potential. Once again, it is often
difficult to determine how much recovery is due to a specific program and
how much would have occurred anyway. Advocates of the status quo and
critics of the innovative tend to be skeptical of the results produced by
innovative rehabilitation programs as phenomena that may have occurred
anyway. The growing base of both scientific and anecdotal evidence
suggests that aggressive rehabilitation programs magnify recovery
potential.
Finally, confounding understanding even further, in
paradigm-expanding speculations, some scientists believe that it is
possible for brain-directed function below an anatomically complete injury
site. For example, Albert Bohbot, whose laserpuncture work was described
previously, believes that there is a sophisticated interaction between our
body’s electromagnetic energy channels/systems/fields and our nervous
system that can bypass the injury site . Although beyond mainstream
biomedical thinking, this is entirely possible under Eastern- and other
esoteric-healing philosophies, and, as such, it has been suggested that
martial-arts study, which emphasize energy-flow and control, would
facilitate this potential.
Summaries are provided below on various
private-clinic and university-based rehabilitation programs that may
restore some function after SCI. The agendas and priorities of the
programs in these two settings often vary greatly. The latter is often
research driven with the goal of publishable professional papers and
awarded grants, and with the former, research by itself is not the goal
but the production of real-world results that economically sustain the
program.
2)
Neuro Institute: Arnie Fonseca (Arizona, USA) summarized his
aggressive physical rehabilitation program at the 2001 Iceland conference
in Iceland (see introduction). An exercise physiologist, Fonseca draws
upon his former coaching experience to motivate clients with SCI and other
neurological disorders to regain surprising function. The author of this
report has met Fonseca and was impressed with his drive, can-do spirit,
and commitment to his rehabilitation mission, a mission that became
personal after his 21-year-old son Brandon sustained a serious head injury
from an auto accident.
Summarized on the Neuro Institute’s website (www.theneuroinstitute.com;
also see www.healingtherapies.info), Fonseca describes his program as
immersion therapy. Basically, he believes that the best way for a
neurologically compromised patient to accrue positive results is to be
immersed in goal-oriented rehabilitation therapy for at least three
hours a day for three to five days a week. There is no magic technique;
the program uses a variety of rehabilitation approaches ranging from
state-of-the-art, sophisticated electronic equipment (e.g., FES bikes) to
old-fashioned, low-tech weight training. Through his “just-do-it”
motivational prowess, Fonesca encourages patients to replace entrenched
defeatist attitudes with a new conviction of what is possible if they work
hard.
A number of impressive success stories are documented
on the Neuro Institute’s website. One of the more notable involves Andrea,
whose experience was discussed earlier under the omental therapy section.
Her experience represents a good example of how function-restoring
surgeries are being combined with aggressive physical rehabilitation. In
brief review, an omental/collagen bridge was used to bridge a 4-cm gap in
Andrea’s cord that resulted from a skiing accident (Neurological
Research 27, 2005). Several years after surgery, Andrea started
Fonesca’s program, and has regained considerable function, including some
ambulatory ability. Time-sequential MRIs indicate ongoing development of
axonal structure through the once huge spinal-cord gap. Although it is
difficult to distinguish surgery from rehabilitation contributions, much
to the chagrin of scientific purists, this is the sort of synergistic
surgical-rehabilitation programs that we are going to see much more of in
the future.

3) The
Project Walk (California, USA) intensive exercise-based
recovery program for SCI was developed by Ted and Tammy Dardzinksi (www.projectwalk.org).
Many individuals with SCI who have committed to this program have accrued
additional function much beyond what was considered possible after injury.
Using the “Dardzinski Method,” the program attempts to re-educate the
damaged nerv ous
system through appropriate physical stimulation. Because each injured
nervous system is unique and each patient, as a result, has different
capabilities, the program is tailored to the client. (Photo: Project Walk
Clinic).
ous
system through appropriate physical stimulation. Because each injured
nervous system is unique and each patient, as a result, has different
capabilities, the program is tailored to the client. (Photo: Project Walk
Clinic).
Briefly, the program focuses on developing muscle
potential below the injury level. The Dardzinksi’s feel that standard
rehabilitation programs not only ignore this potential but contribute to
its extinction by “tossing-in-the-towel” focusing on non-paralyzed body
parts needed for adaptation to wheelchair living instead of ambulation.
They also feel that the extensively administered
anti-spasticity and other movement- and sensation-inhibiting medications
are the equivalent of pouring water on the flickering embers of
regeneration that often still exist after injury. In contrast, Project
Walk’s goal is to fan these embers into a phoenix-like re-emergence of
functionality. As discussed in the introduction to this section, the
program attempts to shift the patient from the all too common
“you-will-never-walk-again” belief that is commonly imprinted by medical
authorities after injury to a self-fulfilling attitude of what could be
truly possible with hard work.
Underscoring their reservations with traditional
rehabilitation principles that are based upon the limitations of the past
than the promise of the future, the Dardzinksi’s note: “If you were to
place an able-bodied person in a reduced gravity environment, tell them
they can’t move for a year, heavily medicate them, and give them no hope,
what do you think the outcome would be? Bone density, muscle mass, and
nervous system activity would begin to shut down and disappear. That
able-bodied person would have the same symptoms of a paralyzed person. So,
is it just the injury or the treatment that keep some SCI paralyzed?”
Like many other SCI programs that believe that there
is a therapeutic window after injury in which the recovery potential is
greatest, Project Walk ideally would like to start treating patients
relatively soon after injury. The program feels that without proper
stimulation and load bearing, a newly injured individual with SCI will
soon start losing bone density, muscle mass, and CNS functioning, which
will make functional recovery in the future even more difficult. Although
the program has treated many after this early therapeutic window,
sometimes with dramatic improvements, much more effort is required to
accrue the same degree of benefit. Nevertheless, the issue of early
treatment represents a bone of contention to many traditional SCI
rehabilitation specialists who often dismiss any improvement as something
that would have accrued anyway during this period of neuronal plasticity.
Although the training schedule varies depending upon
the individual’s function, the average client typically works out three
hours every other day. For people who must return home, individually
tailored, home-based programs are designed. Although the program is
intensive, it encourages clients not to embrace it exclusively at the
expense of overall life balance through career, school, social life, etc.
The program consists of intense one-on-one training
that combines strengthening activities for all muscles in the extremities
and core (abdominal, back, and pelvic), balance work, and coordination
drills. Again, exercise routines are structured to activate paralyzed
areas and strengthen weak muscles. Specialists facilitate active and
passive motions with participants in various planes of motion to
reactivate and reorganize the nervous system. This includes but is not
limited to floor exercises, assisted/unassisted work on Total Gyms®, and
body weight supported ambulation. The common component of these exercises
is weight bearing through the long bones of the body. The program believes
that weight bearing is essential to recovery of function because that is
what the human body was designed to do.
Functional improvements often include increased
muscle mass, CNS activity, health and well being, sensation and function
below the injury level, occupational skills, and sweating, as well as
decreased drug dependence and pain.
The program encourages the use of a
variety of synergistic healing modalities, including
acupuncture,
hyperbaric oxygen therapy, and the use of standing frames, FES bikes
and other external electrical stimulation that helps to maintain muscle
mass and circulation. The program also emphasizes good nutrition.
The recently published results of a non-randomized
study indicate that Project Walk’s intense-exercise regimen generates
substantial functional improvements in individuals with chronic SCI
(Harness ET et al, Spinal Cord, 46, 2008). Representing a good
example of the much needed cooperation between independent clinics
attempting to produce results for patients in real-world settings and
academicians with foremost allegiance to the scientific process, Project
Walk staff worked with University of California Irvine investigators to
document these exercise-generated improvements.
In the study, 21 individuals with chronic SCI (both
cervical and thoracic injuries) who underwent six months of Project
Walk’s intense exercise (IE) program were compared to eight controls
whose program consisted of an unstructured, self-regulated exercise over
the same period. IE and control subjects averaged 38 and 34 years old,
respectively. On average, 3.3 years had elapsed since injury for IE
subjects compared to eight years for controls. Over the study’s
six-month exercise period, IE and control subjects averaged 7.3 and 5.2
hours of exercise per week, respectively.
Before the exercise program was initiated, both
groups had comparable motor function. Compared to controls, those
enrolled in the intense-exercise program improved greatly. Specifically,
71% of IE subjects improved in motor function in contrast to only 25% of
controls (25% of controls also decreased in function). Furthermore, in
one third of the IE subjects, at least one muscle changed from
non-functional to functional after the six months of training.

4) Coordination
Dynamics Therapy was developed by Dr. Giselher Schalow, a
German scientist with programs in Estonia, Spain, and formerly
Switzerland. According to Schalow’s website (http://www.cdt.host.sk/)
coordination dynamics therapy (CDT) was introduced by him for “functional
and structural repair of the lesioned or malfunctioning human central
nervous system (CNS). This mainly movement therapy improves (1) the
self-organization of the neuronal networks of the CNS for functional
repair by exercising extremely exact coordinated arm and leg movements on
a special device and, in turn, the coordinated firing (with respect to
time and space) of the many billions of neurons of the human CNS.
Structural repair is achieved by training automatisms like creeping,
crawling, walking and running and by forcing the ‘adaptive machine’ CNS to
adapt by pushing the patient to the limits during exercise.”
Although underscoring
that it’s the program and not the equipment per se that makes the
difference, the device Schalow emphasizes is a Swiss-manufactured GIGER MD
exercise instrument, which has become popular at many rehabilitation
centers. The patient powers the instrument in either standing, sitting, or
lying-down positions. Arm and leg cycling is phased in a physiologically
sequenced and coordinated pattern that promotes the creation and
reorganization of fun ction-restoring
CNS neuronal networks.
Basically, CDT’s gestalt-like approach to muscle movement
emphasizes the neuronal plasticity (i.e., adaptability) that is inherent
in all. With CDT, it is the rhythm of the exercise patterns not the
exercise itself that is most important. Through a wave-like movement, all
spinal-cord sections are sequentially affected. (Thumbnail photo of
Schalow's clinic: In front a patient with SCI (T-5/6) crawling, supported
by a physiotherapist; a patient with an incomplete SCI jumping on
springboard; a patient with a complete SCI exercising on GIGER MD device;
on the treadmill is a patient with formerly severe brain injury.)
ction-restoring
CNS neuronal networks.
Basically, CDT’s gestalt-like approach to muscle movement
emphasizes the neuronal plasticity (i.e., adaptability) that is inherent
in all. With CDT, it is the rhythm of the exercise patterns not the
exercise itself that is most important. Through a wave-like movement, all
spinal-cord sections are sequentially affected. (Thumbnail photo of
Schalow's clinic: In front a patient with SCI (T-5/6) crawling, supported
by a physiotherapist; a patient with an incomplete SCI jumping on
springboard; a patient with a complete SCI exercising on GIGER MD device;
on the treadmill is a patient with formerly severe brain injury.)
Schalow compares the process to a computer, in which
“the CNS neurons and connections represent the computer’s hardware, and
the many different self-organizations of neural networks activated by
volition and movement-induced input represent the computer’s software.”
With this analogy, no matter how powerful your computer, if the software
(i.e., neuronal circuits and networks) is not there, you are not going to
have significant function. As such, efforts to regenerate neurons without
adequate consideration on how they are organized will be inherently
limited.
To reinforce the creation of these nascent,
function-restoring neuronal networks requires a substantial effort
commitment on the patient’s part; specifically, it is recommended that
patients train 20-30 hours per week for at least a half year. Under this
regimen, the sequenced movements are repeated many thousand of times.
Schalow published his SCI findings in several
professional articles. For example, in 2002, he reported the results of
treating 18 patients with at least three months of CDT (Electromyogr
Clin Neurophysiol, 42). Patient age ranged from 7-55 years old
(averaged 31), and the time since injury averaged five years. In addition
to measuring increased ability to creep, crawl, springboard jump, walk,
and step climb (which was selectively and not cumulatively reported),
Schalow quantified improvements through a “coordination-dynamics”
measurement that reflects CNS organization. After three months of CDT,
this measurement improved 53%, 32%, and 48% for patients with cervical,
thoracic, lumbar injuries, respectively. Given the results, Schalow
suggested that cervical and lumbar injuries have greater plasticity
potential (i.e., adaptability) than thoracic injuries. Overall, motor
function improved in all patients.
In 2003, Schalow reported the results of treating
four patients with CDT for longer 6-13-month periods (T12/L1, C4/5 injury,
T12, and L3/4 injuries) (Electromyogr Clin Neurophysiol, 43). Three
were from the previously reported group. The article concluded: “One
patient with an incomplete spinal cord lesion was cured, two patients with
clinically complete injuries were partly cured, and one patient with a
complete spinal injury L3/4 became incomplete but showed only comparably
little progress.”

5) Activity-Based
Restoration: Dr. John McDonald, who recently shifted his
program from St. Louis’ Washington University to Baltimore’s Johns Hopkins
University, has developed an “activity-based restoration” (ABR) program
that reinforces patterned neural activity, which, in turn, promotes the
creation of function-restoring neuronal networks.
 ABR
is based on the premise that there is often considerable neuronal
plasticity (i.e., adaptability) that can be exploited after injury but
generally has not been under conventional rehabilitation. In most, even
clinically classified complete, injuries, there are substantial numbers of
intact neurons that still cross the injury site. Through rigorous
physical stimulation, these residual neurons provide the foundation for
creating new function-restoring neuronal networks.
ABR
is based on the premise that there is often considerable neuronal
plasticity (i.e., adaptability) that can be exploited after injury but
generally has not been under conventional rehabilitation. In most, even
clinically classified complete, injuries, there are substantial numbers of
intact neurons that still cross the injury site. Through rigorous
physical stimulation, these residual neurons provide the foundation for
creating new function-restoring neuronal networks.
It is an “if-you-don’t-use-it-you-lose-it” system, in
which paralysis-associated disuse of muscles over time results in a
viscous-circle diminution of regeneration potential. In other words, the
nervous system requires a certain degree of pattern activity to maintain
itself. As such, dormant neurons and nascent neuronal networks somehow
must be stimulated, even in the case of paralysis. Like others, McDonald
believes that one’s inherent adaptive potential in response to patterned
activity is severely compromised by commonly used anti-spasticity
medications.
In McDonald’s ABR program, the pattern-activity
stimulation is primarily from training on a recumbent
functional-electrical-stimulation (FES) bicycle for one hour three times a
week.
 This
one-hour effort corresponds to about 3,000 repetitions, which compares to
the 12,000 steps the average person takes each day. With this FES device,
the computer-controlled, muscle-stimulating electrodes were attached to
the skin over the quadricep, hamstring, and gluteal muscles. Supplemental
therapies included the corresponding electrical stimulation of other
muscle groups, as well as aqua-therapy after some recovery has accrued.
Because of the need to maintain a three-session-per- week schedule, to
make the program feasible for most individuals, McDonald feels that it
ideally should be home based with monitoring over the Internet.
This
one-hour effort corresponds to about 3,000 repetitions, which compares to
the 12,000 steps the average person takes each day. With this FES device,
the computer-controlled, muscle-stimulating electrodes were attached to
the skin over the quadricep, hamstring, and gluteal muscles. Supplemental
therapies included the corresponding electrical stimulation of other
muscle groups, as well as aqua-therapy after some recovery has accrued.
Because of the need to maintain a three-session-per- week schedule, to
make the program feasible for most individuals, McDonald feels that it
ideally should be home based with monitoring over the Internet.
McDonald’s program accrued considerable visibility
after the late actor Christopher Reeve regained some astonishing,
unexpected function after starting ABR five years after injury, i.e.,
well into the chronic phase of injury in which, from historical
rehabilitation perspectives, the probability of significant functional
recovery is considered unlikely. Reeve’s improvements were documented by
McDonald et al in a 2002 article (J Neurosurg (Spine 2), 97).
Forty-two years old at the time of his injury in
1995, Reeve sustained an ASIA Grade-A complete C-2 injury after being
thrown from a horse. Five years later, Reeve started the ABR program and
continued it at home. In spite of his clinically classified complete
injury, as is the case with so many injuries, magnetic-resonance imaging
indicated that Reeve had a doughnut-like rim of tissue (~25% of the normal
amount of spinal-cord tissue) surrounding a injury-site cyst.
After three years of treatment, Reeve improved from
ASIA Grade-A classified complete injury, which had been his status for the
five years before treatment, to Grade-C incomplete injury (again, as
described in appendix, this impairment scale ranges from Grade A,
representing complete injury, to Grade E, representing normal motor and
sensory function). Over his three-year treatment period, Reeve’s motor
scores improved from 0 on a scale of 0-100 to 20, and sensory scores
improved from 5-7 on a scale of 0-112 to 55-77. These improvements
correlated with a regained ability to move certain muscles, including most
joints in gravity-countering water. Sensation as measured by pinprick and
light-touch evaluation improved to 50% and 66% of normal, respectively.
This recovery was also associated with a reversal of SCI-associated
osteoporosis, increased muscle mass, a greatly reduced incidence of
antibiotic-requiring infections and other medical complications, and
reduced spasticity.

6)
Shepherd Center’s Beyond Therapy Program
(Atlanta, GA) is designed to integrate the goals of each client into an
individualized program that combines the principles of athletic training
along with concepts of traditional physical therapy to promote spinal-cord
neural recovery. Recent research suggests that the central nervous
system, once thought to be irreparable, is actually able to functionally
reorganize itself with the appropriate training and may allow recovery of
lost abilities even in the presence of minimally intact neural tissue.
The program’s
vision is to create an environment of hope and determination for those
clients who have sustained a catastrophic neurological injury and provide
them with the appropriate assistance to achieve their highest level of
sensory and motor recovery. It is designed to challenge clients to reach
a level of physical fitness or function that they had once thought
impossible. The program works to change the focus of the client’s mindset
away from the wheelchair and toward rehabilitation and recovery. Goals
include stimulating intact spinal-cord neural tissue that was spared
during the initial injury to promote neuromuscular recovery, facilitating
neural recovery in individuals who have undergone experimental
function-restoring surgeries and therapies throughout the world, and
creating an individualized lifelong activity program to help individuals
maintain physical readiness for neural recovery.
Beyond Therapy is a physically rigorous program that
combines the expertise of an individualized training team comprised of
exercise physiologists, athletic trainers and physical therapists to
assist their clients in attaining the highest level of personal strength
and restoring function. Because this program integrates multiple
disciplines, there are no boundaries in the variety of experiences and
stimuli that clients may receive. The program extends beyond the range of
acute care and predetermined functional goals, and continues the
rehabilitation process by administering aggressive treatment of clinically
researched protocols to achieve a higher-level of individual
achievement.
Clients are first evaluated by a physical therapist
who designs an intense 9-hour/week program that combines state-of-the-art
technological advancements in rehabilitative medicine with hard-core
physical training. Each client is evaluated to determine the most
appropriate individualized training program which may include the
following: Lokomat (Robotic assisted treadmill training),
body-weight-support manual treadmill training, Giger training, FES
(functional electrical stimulation) bike training, Bioness upper extremity
orthotic electrical stimulation, aquatic therapy, standing and gait
training with a variety of orthosis/equipment, lower extremity
strengthening, upper body and core strengthening in a variety of
developmental sequencing techniques.
Beyond Therapy’s philosophy originates from three
primary concepts. The first is recovery through the use of neural
patterned activity. The client is able to use the most technologically
advanced equipment to take their bodies safely through the normal movement
patterns and weight bearing that they completed on a daily basis before
their injury to remind and re-teach their damaged nervous system how to
function appropriately. This may include timed walking on the Lokomat,
cycling on an FES Bike, or passive/active cycling with a Giger MD. The
second concept is that of task specificity. The injured nervous system
responds to training and has the ability to modify activity based on the
specific training program or inputs that it receives. This includes
teaching the injured nervous system specifically how to crawl and stand
again as individual components of their recovery process. The third
concept is that of functional strengthening. All four limbs and core must
be strong enough to support the body’s weight to complete the activity
demands being placed upon it by a healing nervous system.
Beyond Therapy’s experimental protocol
was designed to assist clients with navigating through the neurological
experimental procedures offered at Shepherd and throughout the world.
This program assists those clients who wish to pursue innovative
procedures around the world and need information on how to participate in
them.

7) The
Rehabilitation Institute of Michigan’s Center for Spinal Cord Injury
Recovery (CSCIR) is designed to implement and study the results
of innovative treatments that may result in some functional improvement in
persons with SCI. To maximize restored function, the program has
rehabilitated numerous patients who have undergone various
function-restoring cell/tissue-transplantation procedures, including those
previously discussed [e.g., Dr. Carlos Lima (Portugal), Dr. Hongyun Huang
(China), Dr. Bryukhovetskiy (Russia)].
Basically,
CSCIR offers long-term,
high-intensity, state-of-the-art, outpatient therapy that focuses on
neuromuscular recovery. The program incorporates therapeutic techniques
based on the updated information available from emerging research around
the globe. The team works one-on-one with clients to develop creative,
individualized therapeutic exercise programs targeted at improving
movement and sensation. The program emphasizes neuromuscular
re-education, sensory stimulation, weight-bearing exercise, functional
electrical stimulation (FES), aquatic therapy, hand therapy, and massage.
The CSCIR program moves beyond traditional rehabilitation techniques and
focuses on activating muscles and nerves above and below the level of
injury that can develop into movement, sensation, posture,
balance, and coordination improvements.

8)
Drs. Carlo Alberto Arcangeli and Giovanna
Lazzeri at the Centro Giusti
Rehabilitation Center (Florence, Italy) have developed an intensive
rehabilitation program which has restored function to many individuals
with SCI (www.centrogiusti.it).
The program has provided follow-up
rehabilitation to Dr. Carlos Lima’s patients who have had, as previously
discussed, olfactory tissue transplanted back into their injured spinal
cord.
The program’s overall philosophy
is that post-injury recovery is greatly enhanced by the stimulation
provided by ongoing, rigorous physical rehabilitation. The goal is to
stimulate every possible improvement, however small it may be, thus
validating all physical, mental, and economical efforts. The patient must
understand that the work involved is “active” on his part, albeit
with the assistance of a therapist and limited aids (too much of such
assistance makes the exercises passive and, therefore, lacking
stimulation). Given these considerations and having the Russian
Rehabilitation School as a background, Drs.Arcangeli and Lazzeri have
developed the Intensive Continual Motor Rehabilitation Program R.I.C.
The program has produced
functional improvements in numerous patients with SCI. For example,
patients with complete cervical injuries have regained a dynamic standing
position; many patients with paraplegic, even complete, injuries are now
walking with a small orthosis below the knee, simple gait trainer, and
therapist assistance; and many with tetraplegic, including complete,
injuries after toning up the area above the injury have regained various
functions, including walking with orthosis aid, gait trainer and therapist
assistance. Numerous patients have reached their goal of virtually
abandoning their wheelchairs, challenging their original diagnoses.
With this program, Dr. Lima’s
olfactory-tissue-implantation patients can be compared to patients who
have not undergone the procedure, providing new clinical opportunities to
be obtained through rehabilitation. They are showing functionality far
beyond what could have been expected, e.g., active movements below injury
and superior physiological deambulation (i.e., walking about).
The program’s objective is to
stimulate the patient to continue to discover improved movement, which, in
turn, evolves into functional movements such as deambulation. The program
consists of up to 150 exercises (carried out in various postures) that
work toward maximizing potential, coordination, balance, posture, and body
recognition. Because the exercises are actively carried out, considerable
motivation and will are necessary.
The program is distinguished by
its intensity, continuity, and personalization. 1) Intensity: The
program consists of 4-6 hours, five-days a week, therapist-assisted
sessions. 2) Continuity: Program duration cannot be determined in
advance. The first three months are spent in the center, followed by 5-6
months at home, and then three weeks again at the center. At home, the
patient must be followed by a program-trained therapist and must have the
necessary program apparatus. The patient will then carry on alternating
home with center therapy for three-week periods. With this organization,
the program evolves over time. 3) Personalization: The program is
personalized according to the patients’ capabilities and clinical
situation. The patient-therapist relationship is always on a 1-1, or even
1-2, basis.
Through intense stimulation above
and below the injury level, combined with strong motivation, the body’s
natural physiological resources are used. Recovery is due to a variety of
events, such as the reactivation and use of various muscle groups above
the injury that would not otherwise be used, the activation of the
bone-marrow structure below the injury, and numerous other unexplored body
resources. The main objective is to regain a physiological deambulation
that is as independent from aids as much as possible during which many
other secondary goals are reached, such as regaining muscular potential,
lost functions, obtaining a standing and dynamic position, some transfer
independence, balance, coordination, postural control, and prevention of
various immobility-related side effects, such as osteoporosis.
Deambulation is taken into consideration only when the patient is able to
maintain good standing-position trunk balance and is not considered an
exercise but an end result and reassembling of the exercises. Complete
body weight must be put onto the lower limbs while deambulating so that a
realistic biofeedback is given (in contrast to in-water training where the
patient carries out movements but fails to repeat movements when on
ground).
To prevent the “collapsing of the
building,” a solid foundation (muscular, articular (i.e., joints), body
recognition, and emotional) must be built up before attempting
deambulation. From a psychosocial viewpoint, the patient feels sure of
himself in his movements; i.e., he feels “alive,” busy, motivated, and
stimulated in enjoying a better societal position. When working on the
body, program staff believes that they are also working on the psyche.
TOP